Understanding recovery process could have implications for many different injuries of the central nervous system
An interdisciplinary team of University neuroscientists and neurosurgeons has used a new imaging technique to show how the human brain heals itself in just a few weeks following surgical removal of a brain tumor.
In a study featured on the cover of the current issue of the journal Science Translational Medicine, the team found that recovery of vision in patients with pituitary tumors is predicted by the integrity of myelin—the insulation that wraps around connections between neurons—in the optic nerves.
“Before the study, we weren’t able to tell patients how much, if at all, they would recover their vision after surgery,” explained David Paul, an M.D. candidate in the Department of Neurobiology and Anatomy, and first author of the study.
When pituitary tumors grow large, they can compress the optic chiasm, the intersection of the nerves that connect visual input from the eyes to the brain. Nerve compression can lead to vision loss, which usually improves after these tumors are surgically removed.
Paul and his colleagues used a technique called diffusion tensor imaging (DTI) to show how changes in a particular bundle of nerve fibers relate to vision changes in these patients.
“DTI measures how water spreads in tissue,” explained Bradford Mahon, assistant professor in the Department Brain and Cognitive Sciences and the Department of Neurosurgery, and senior author of the study. “The myelin insulation normally prevents water from spreading within the nerves, which would cause the nerves to malfunction.”
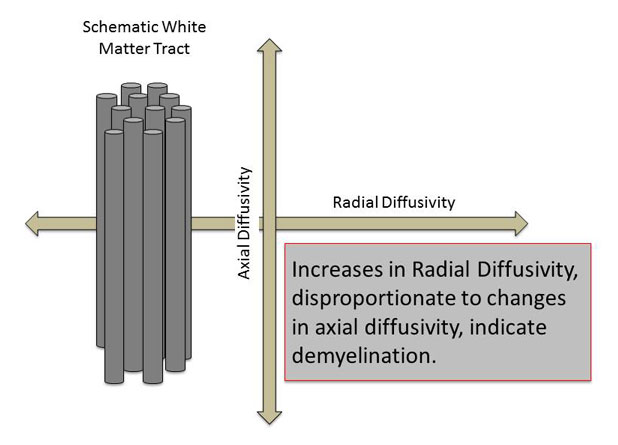
Paul described myelin damage by analogy to an insulated copper cable. In the human brain, DTI can measure the “leakiness of the insulation,” or how well myelin constrains the flow of water in brain tissue.
One DTI-based measurement, called radial diffusivity, can be used as an indicator of myelin insulation; an increase in this measure means there is less insulation to restrict the movement of water within a nerve. In their study, the researchers found that inadequate insulation resulted in poorer visual ability in patients.
Paul said this particular patient population is unique because unlike other diseases such as stroke, trauma or multiple sclerosis, these patients have a problem that can be treated by surgery and the effect of the tumor on the brain is the same every time. Every pituitary tumor that grows large enough will compress the optic chiasm in more or less the same place, and removal of the tumor is often followed by a recovery of visual abilities.
“These patients grant us a unique opportunity to understand human brain repair because the surgery is minimally invasive and patients recover very quickly after surgery,” said Edward Vates, director of the Pituitary Program in the Department of Neurosurgery at the University of Rochester Medical Center, and co-author of the study.
The measurements established in the study provide a new way to measure the structural integrity of nerve fibers, and may ultimately be applicable across the full range of brain diseases and injuries.
“There’s a lot of variability in how people recover from brain injuries,” said Mahon. “Anything we can learn about patients who go on to make a good recovery may help us to promote recovery from brain injury of any cause.” He added that the visual system is the best understood circuitry in the human brain, and his lab has developed very precise ways of studying vision before and after surgery.
“If we can develop our prognostic methods in the context of the early visual pathway, then we can apply the same types of models to more complex systems in the brain, like language recovery after a stroke,” said Mahon.
“This kind of research will create novel treatments to fix broken nervous systems,” said Bradford Berk, director of the new University of Rochester Neurorestoration Institute. “Harnessing new technologies to help us understand how the brain repairs itself and restores function, and how we can accelerate that process will be one of the keys to restoring neurological function in a wide range of conditions, such as multiple sclerosis, stroke, and traumatic brain injury.”
Additional researchers on the study are Elon Gaffin-Cahn, Eric B. Hintz, Giscard J. Adeclat, and Zoë R. Williams from the University of Rochester/University of Rochester School of Medicine, and Tong Zhu from the University of Michigan Medical Center.
The National Institute of Neurological Disorders and Stroke, the National Eye Institute, and the National Center for Advancing Translational Science supported the study. David Paul received additional support from the CTSI Pre-Doctoral Training Program at the University of Rochester Medical Center.



