In Review
Nerve Cells Key to Making Sense of Senses
 PARALLEL PROCESSING: Neurons firing in the brain. (Photo: Jonathan Clarke/Wellcome Images)
PARALLEL PROCESSING: Neurons firing in the brain. (Photo: Jonathan Clarke/Wellcome Images)How does the human brain manage all the sensory information it receives from the eyes, ears, nose, mouth, and skin? New research by a team of scientists from Rochester, Washington University in St. Louis, and Baylor College of Medicine suggests that the answer lies in a relatively simple computation performed by single nerve cells, an operation that can be described mathematically as a straightforward weighted average.
Published online in Nature Neuroscience, the study represents the first direct evidence of how the brain combines multiple sources of sensory information to form as accurate a perception as possible of the environment. The discovery may eventually lead to new therapies for people with Alzheimer’s disease and other disorders that impair a person’s sense of self-motion, says study coauthor Greg DeAngelis, professor and chair of the Department of Brain and Cognitive Sciences.
The study confirms and extends a computational theory developed earlier by Alexandre Pouget, a brain and cognitive scientist at Rochester and at the University of Geneva in Switzerland and a coauthor of the new paper. According to the theory, neurons fire in a manner predicted by a weighted summation rule. While that was largely confirmed by the study’s data, the neurons followed a pattern that was slightly off target from the predictions, a difference that could explain why behavior also varies slightly among subjects, the authors conclude.
“Being able to predict these small discrepancies establishes an exciting connection between computations performed at the level of single neurons and detailed aspects of behavior,” says DeAngelis.
—Susan Hagen
Age a Big Factor in Prostate Cancer Deaths
Contrary to common belief, men age 75 and older are diagnosed with late-stage and more aggressive prostate cancer and thus die from the disease more often than younger men, according to a Rochester study published in the journal Cancer.
The study is particularly relevant in light of a recent controversy about prostate cancer screening. In October, a government health panel said that healthy men age 50 and older should no longer be routinely tested for prostate cancer because the screening test in its current form doesn’t save lives and sometimes leads to needless suffering and overtreatment. Patient advocates and many clinicians disagreed with the finding.
“Especially for older people, the belief is that if they are diagnosed with prostate cancer, it will grow slowly, and they will die of something else,” says lead author Guan Wu, assistant professor of urology and of pathology and laboratory medicine. “We hope our study will raise awareness of the fact that older men are actually dying at high rates from prostate cancer. With an aging population, it is important to understand this, as doctors and patients will be embarking on more discussions about the pros and cons of treatment.”
—Leslie OrrResearchers Identify Health Disparities with Deaf ASL Users A new study conducted by Rochester researchers represents the first time a deaf community has used its own data to assess its health status.Using communication tools that enabled deaf people to identify health priorities, the study—published in the American Journal of Public Health—found higher rates of obesity, partner violence, and suicide but lower rates of smoking than in the general population. Traditionally, deaf people who use American Sign Language (ASL) are excluded from health research and thus are medically underserved, the study noted. “This is a monumental step toward eliminating health disparities and advancing the health of deaf people,” says Thomas Pearson, the Albert D. Kaiser Professor in the Department of Community and Preventive Medicine. He directs the Clinical and Translational Science Institute and the National Center for Deaf Health Research at the Medical Center. The University has worked with community partners to apply successfully for research grant funding to address three health priorities identified by the study: obesity, suicide risk, and violence. —Leslie Orr
 (Photo: Steve Boerner for Rochester Review)
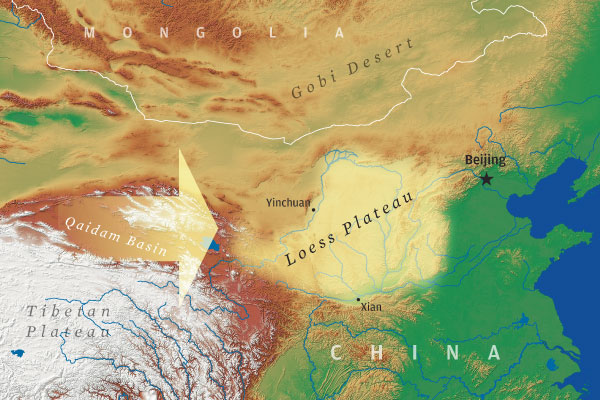
(Photo: Steve Boerner for Rochester Review)New Sources Found for Accumulated Dust on Chinese Loess Plateau
Geologists have long thought that the loess—or fine silt—that accumulated on the Chinese Loess Plateau was carried on winds from desert regions to the northwest over the past 2.6 million years. But new research indicates the loess may actually have come from due west, which would change conventional thinking about wind patterns during that period.
A Rochester-led team of geologists from the United States and China compared the composition of uranium and lead in zircon crystals excavated from the plateau and potential source sites. The scientists found that the ages of the crystals from the Chinese Loess Plateau matched with samples from the northern Tibetan Plateau and the Qaidam Basin, both of which are due west.
“The research should help us better understand how the earth behaves as a system,” says lead author Alex Pullen, a postdoctoral associate in earth and environmental sciences. “With that knowledge, we’ll be able to improve our climate models.”
The results were published in the journal Geology.
—Peter Iglinski
Medical Center Awarded Patents
Cervical Cancer Vaccines
The University has been awarded a U.S. patent for research essential to both human papillomavirus vaccines on the market. The patent recognizes the work by three University virologists—Richard Reichman, William Bonnez, and Robert Rose ’94M (PhD)—who were the first to demonstrate that HPV virus-like particles, a harmless mimic of the infectious virus with no risk of infection, provoke a protective immune response against the types of HPV that cause cervical and oropharyngeal cancer. The Rochester technology has been incorporated into Gardasil and Cervarix, two vaccines approved for use against HPV.
‘Living Chip’ Technology
The Medical Center has also received a patent for a medical device that could revolutionize the way that physicians monitor the health of their patients. The device—which consists of an implantable “living chip”—is designed to give doctors real-time information about their patients’ health and, more importantly, alert them to changes in their conditions. Spencer Rosero, associate professor of medicine and director of the Pacemaker Clinic, developed the technology behind the device.
—Tom Rickey and Leslie White

